Hives
Aurora Dermatology now offers bulk-billed phototherapy for chronic hives (urticaria).
Ask us today.
What are hives (urticaria)?
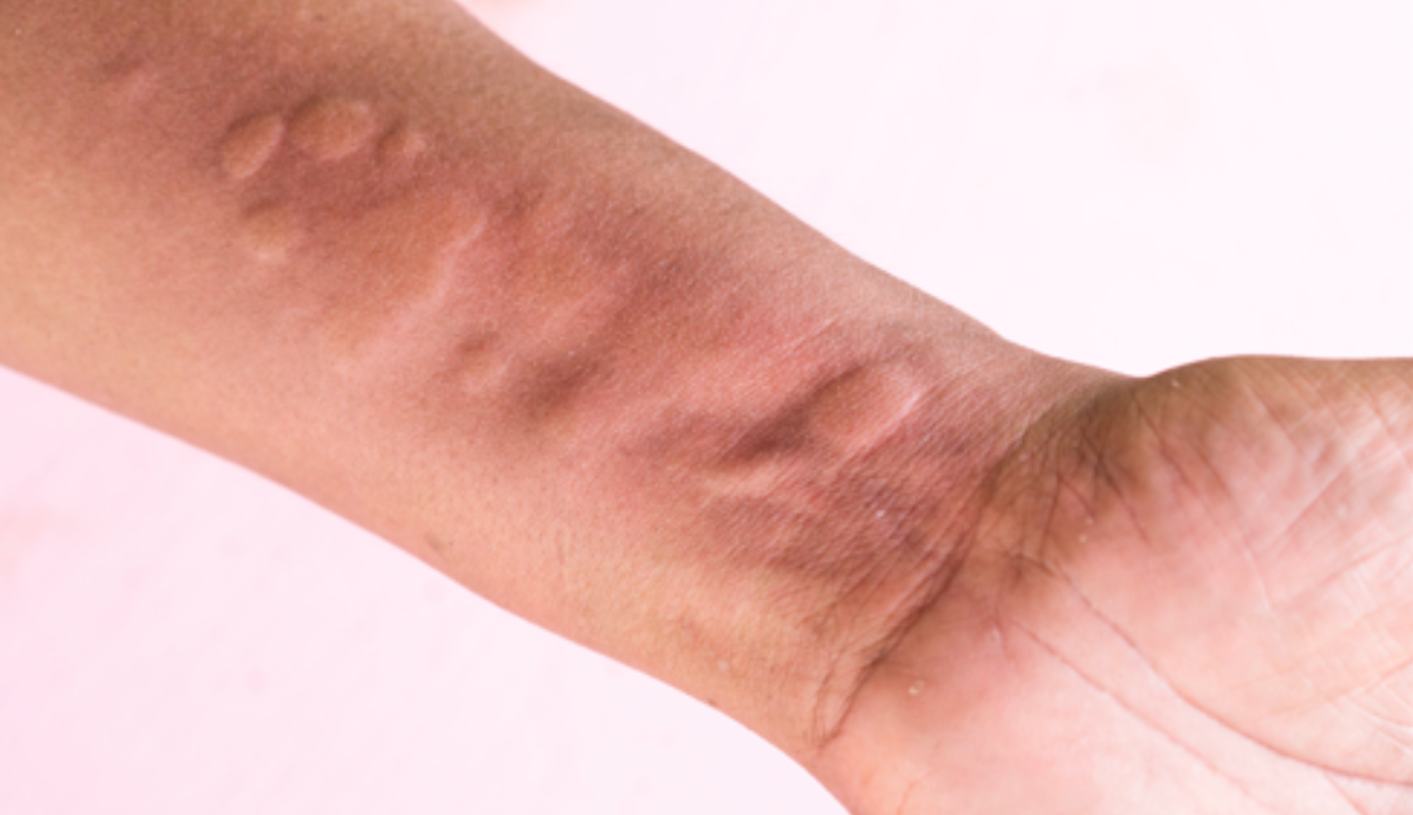
- Hives, the layman’s term for urticaria, are pink or red, itchy rashes that may appear as blotches or raised round lumps (called weals) on the skin.
- They can range from the size of a pinhead, through to a pea or a small dinner plate and often are mistaken as mosquito bites.
- Swellings typically disappear within minutes to hours in one spot, but may come and go for extended periods – sometimes weeks at a time.
- Hives can be classified as acute (less than 6 weeks) or chronic (greater than six weeks) with daily or episodic weals.
How common are hives?
- Hives are very common impacting about 20% of people in their lifetime.
- Hives affect all races and both sexes.
Aurora Dermatology now offers bulk-billed phototherapy for chronic hives (urticaria). Ask us today.
What are the symptoms of hives (urticaria)?
- Hives or weals can be a few mm or several centimetres wide.
- A telltale sign of a hive is that it blanches (becomes paler) when pressed in the middle.
- Hives can be white or red, with or without a red flare.
- They can be round, form rings or giant patches.
- Hives can affect any site of the body and can be widely distributed.
- Hives can also cause deeper swellings in the skin and mucosa and this is called angioedema.
- These swellings are often larger, may itch less, may burn and respond less well to antihistamines. This type of urticaria most frequently impacts the lips and face.
- Although hives of the face can be embarrassing they are not usually dangerous.
- Acute hives are also often the first sign of a Covid-19 infection.
- Rarely, serum sickness caused by a blood transfusion can cause hives.
What triggers hives?
- It is a common misconception that all hives are due to an “allergic reaction” as MOST hives in children for instance are related to infection.
- Underneath the lining of the skin and organs are mast cells that contain histamine. When these are released into the skin they irritate nerve endings prompting the urge to itch, leak fluid and become red and swollen.
- This reaction can be caused by infection most commonly, or less commonly contact allergies (bee or wasp stings), food allergies (milk and peanuts), or contact allergies for instance latex.
- Wearing unwashed new clothing (textile dermatitis) that contain dyes can also cause a rash and hives.
- A single or recurrent episode of angioedema may be caused by ACE inhibitor drugs, used to treat high blood pressure and heart problems.
Who gets hives and how do they present?
- Hives are uncommon in newborns.
- Inhaled allergens (animal dander, grass, dust) may cause hives and these allergic hives tend to occur within one to two hours of exposure and disappear within six to eight hours.
- Common allergic food triggers for hives include milk, eggs, peanuts and shellfish.
- Antibiotics are also often a medication linked to hives, along with aspirin and ibuprofen, opiates or vaccinations.
- Contact irritants such as saliva or plants such as stinging nettle can also cause hives.
- In adults, urticaria is usually idiopathic and spontaneous but the above food drug and plant triggers can also apply.
- Hives are often common for women around menopause as a result of hot flushes and night sweats.
What are the different types of urticaria?
Dermographism – caused by stroking or scratching the skin, tight clothing, or towel drying after a hot shower.
Cold urticaria – caused by cold water, ice, cold air or cryotherapy (and can be potentially dangerous when swimming due to dizziness).
Cholinergic urticaria – caused by sweat, exercise, emotional distress and hot showers.
Contact urticaria – caused by allergens, white flour, cosmetics, textiles, saliva, meat, fish, vegetables, pseudoallergens or irritants such as stinging nettle, medicines and hairy caterpillars.
Pressure urticaria – Pressure caused several hours earlier from carrying heavy bags, seatbelt pressure, sitting on a horse, standing on a ladder.
Solar urticaria – caused by sun exposure, often spares face, neck hands
Vibratory urticaria – caused by jackhammer
How are hives diagnosed at Aurora Dermatology?
- Dr Parisa will take an extensive history considering family history, previous personal history of skin conditions and allergens and drugs.
- Skin prick tests may be required if allergens are suspected.
- There are no routine diagnostic tests for chronic urticaria, though Dr Parisa may perform a full blood count and C-Reactive Protein test (CBC, CRP) to see if there are underlying disorders.
- Other investigations may be carried out for patients with fever, joint or bone pain and fatigue or other symptoms Dr Parisa may wish to test for. This can also include tests for autoinflammatory disease and urticarial vasculitis.
What is the treatment for hives (urticaria)?
Whilst most urticaria resolves within a couple of weeks with no treatment, the following may be useful.
- Avoid tight clothing and heavy layers in bed at night, spicy foods or alcohol.
- Apply sunscreen to avoid solar urticaria.
- For pressure urticaria, avoid carrying shopping bags, use a trolley instead.
- For cold urticaria, avoid swimming in cold water.
- Take antihistamines
- Failure to respond to antihistamines after four weeks warrants a referral to a dermatologist., immunologist or medical allergy specialist. Although the outlook for hives is often good and many people grow out of them, up to 15% continue to have wealing at least twice weekly after two years.
- Aurora Dermatology also now offers bulk-billed phototherapy (light therapy) for hives that are chronic. Click here to learn more about Phototherapy.
- This usually requires 12 weeks of quick sessions in the light box. Find out more here.
- When hives are severe, corticosteroids may help relieve itch and for milder hives an over the counter corticosteroid cream may help.
- Sometimes hives can be a challenge to treat if antihistamines fail, and your dermatologist may need to prescribe medications like cyclosporine or hydroxychloroquine that work to calm down the immune system.
- Special diets rarely have a big role to play in the management of hives. However where food allergy is suspected, an elimination diet under medical supervision is advised.
- Note that systemic treatments should be best avoided in pregnancy and breastfeeding, although there have been no reports of birth defects so if treatment is required Dr Parisa will prescribe the lowest risk drug for your condition.
- In severe and chronic hives Omalizumab may be prescribed.
- Omalizumab is a recombinant humanized IgG1 monoclonal antibody that specifically targets human immunoglobulin E (IgE).Mast cells and basophils are specific cells of the immune system that contain histamine and heparin. As soon as IgE binds to an IgE receptor it causes the release of histamine and heparin from the cell.Omalizumab works by inhibiting the binding of IgE to IgE receptors on mast cells and basophils.

