Frontal Fibrosing Alopecia
What is frontal fibrosing alopecia?
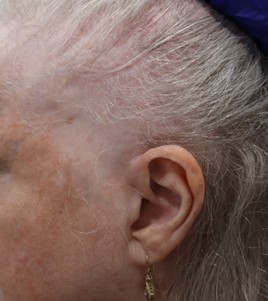
- Frontal fibrosing alopecia is frontotemporal recession of the hairline and eyebrow hair loss, usually in postmenopausal women
- It is associated with perifollicular erythema (redness around the follicle of the scalp), especially along the hairline.
- Frontal fibrosing alopecia is considered a variant of lichen planopilaris, a chronic inflammatory condition affecting skin and mucosal surfaces, but in this case affects the hair.
What are the first signs of frontal fibrosing alopecia?
- A uniform linear band of hair loss along the front and sides of the scalp
- You may notice forehead or other skin areas that have no sun damage.
- Skin may be shiny, pale or mildly scarred without visible hair follicle openings
- The hair pull test is negative (the test where doctor pulls five or six hairs to test for active hair loss).
- Isolated hairs may persist in the bald area – known as the lonely hair sign.
- There is often accompanying eyebrow thinning or madarosis.
- Lesser numbers of patients will have complete hair loss from under arms, pubic hair and limbs.
- For men, sideburns and beard may be involved, sometimes the only area involved.
- Itch and pain may occur in early stages.
- Facial rashes are another early sign (forehead and temples).
- Diffuse redness or red dots around the hairs
- Typical patterns include a diffuse zigzag pattern.
- In men, FFA is commonly misdiagnosed as male pattern baldness.
What is the cause of frontal fibrosing alopecia?
Causes of these conditions include:
- Genetics
- Hormonal changes of post-menopausal patients
- The condition is frequently reported in patients with other comorbid conditions such as hypothyroidism, Type 2 diabetes and autoimmune diseases such as lupus and rheumatoid arthritis.
- Contact allergy to perfume, moisturisers, sunscreen, hair dye remain unconfirmed but possible factors.
How common is frontal fibrosing alopecia and who gets it?
- The incidence of androgenic alopecia (male pattern baldness) impacts more than 50% of men over 50 years, and many women as well after menopause.
- FFA was first reported in 1994, and subsequently, reports of this diagnosis have continued to increase [1,2].
- In a multicenter, retrospective study that included patients evaluated in specialist hair clinics in Europe, America, Africa, and Australia, FFA accounted for 11 percent of 3133 diagnosis of alopecia and 40 percent of 840 diagnoses of cicatricial alopecia [3].
- FFA appears to be an adult-onset disorder; the disorder has not been reported in children. FFA is most frequently diagnosed in postmenopausal women between 55 and 70 years of age but may also occur in other adults [4,10].
- In one of the largest series, a Spanish, multicenter, retrospective study, 83 percent of 355 patients with FFA were postmenopausal women [4].
- Premenopausal women and men accounted for 14 and 3 percent of the patients, respectively. However, a review of 20 patients with histopathologically confirmed FFA in a single center in South Africa found a contrasting distribution; the patients included 5 postmenopausal women, 14 premenopausal women, and 1 man [7].
How is frontal fibrosing alopecia diagnosed?
- Usually, frontal fibrosing alopecia is slowly progressive although it is self-limiting in most cases after several years, with the hair line receding on average of 1.8-2.6 cm.
- As it is a scarring alopecia, hair does not grow back; so it’s important to prevent further hair loss with early treatment and diagnosis.
Is alopecia (areata) the same as frontal fibrosing alopecia?
- Whilst both conditions cause hair loss, alopecia areata is more common in younger individuals and presents as round patches of normal looking skin and hair may grow back because it is not a scarring alopecia.
- FFA is much more common in women over 50 and presents as band-like hair loss.
- It is a scarring alopecia and hair will never grow back.
What is the best hairstyle for frontal fibrosing alopecia and other types of hair loss in women?
- “An asymmetrical parting with a deep side parting can make a sweeping fashion statement and also conceal receding hairlines for the ladies’ ‘, says celebrity hairstylist and one of Huffington Post’s top global beauty influencers for the over 45s Mary Zavaglia
- “Clever styling with headbands, scarves and hats can also disguise hair loss. As can long, thick bangs, a line bob or a jagged layered fringe or even layers around the face.
- “Half up or half down is good if there is receding hairline at the temples (as some of the down hair can disguise missing hair), while a deep side part (the further back from the rear) can also help.”
- Styling with scarves and headbands is also an effective way to reduce a high forehead or thinning hairline, she says.
- You can also use eyeliner or mascara to add extra density to thinning levels of hair.
Hair loss can cause huge psychological devastation and one study from the Royal Australian College of General Practitioners (RACGP) found that 52% of women were “extremely upset” by baldness, compared to 28% of men – with more than 40% of women experiencing marital problems and 64% career difficulties attributed to their hair loss.
Source: https://www1.racgp.org.au/ajgp/2018/july/female-pattern-hair-loss
What is the treatment for frontal fibrosing alopecia?
There is no single effective treatment for frontal fibrosing alopecia.
However, the following treatments may help you retain the hair that remains.
However, the following treatments may help you retain the hair that remains.
These include:
- A short course of oral steroids/injections (either injected into the scalp or as a cream to use at home); this can help with eyebrow hair loss particularly.
- Anti-inflammatory antibiotics to reduce inflammation or anti-malarial tablets
- Finasteride or dutasteride taken as a pill to prevent more hair loss (but should not be used if pregnant).
- Laser therapy for frontal fibrosing alopecia has been shown to be useful light-emitting diodes (LEDs) therapy ,Nd:YAG nonablative laser was reported as an effective method to improve disease symptoms
- Platelet-rich plasma (PRP) injection was reported to achieve stabilization of hair loss and improvement of hairline recession in FFA patients, which showed noticeable positive results.
- JAK inhibitors have been used on other types of non-scarring alopecia (such as alopecia areata) but have not been currently approved for FFA. Some studies showed the efficacy of tofacitinib.
- Biologic medication such as Tildrakizumab (interleukin-23 monoclonal antibody) was administered to a recalcitrant FFA patient who had not responded to various topical and systemic medications.
- Immunosuppressants such as methotrexate, cyclosporin, azathioprine are used for severe and active FFA may be helpful.
- Oral minoxidil can help to keep and increase the density of remaining hair.
- The pioglitazone tablet, Naltrexone tablet, and Bimatoprost cream used in some patients has had successful results.
- Isotretinoin tablets can improve facial papules in patients with FFA but do not improve hair loss.

