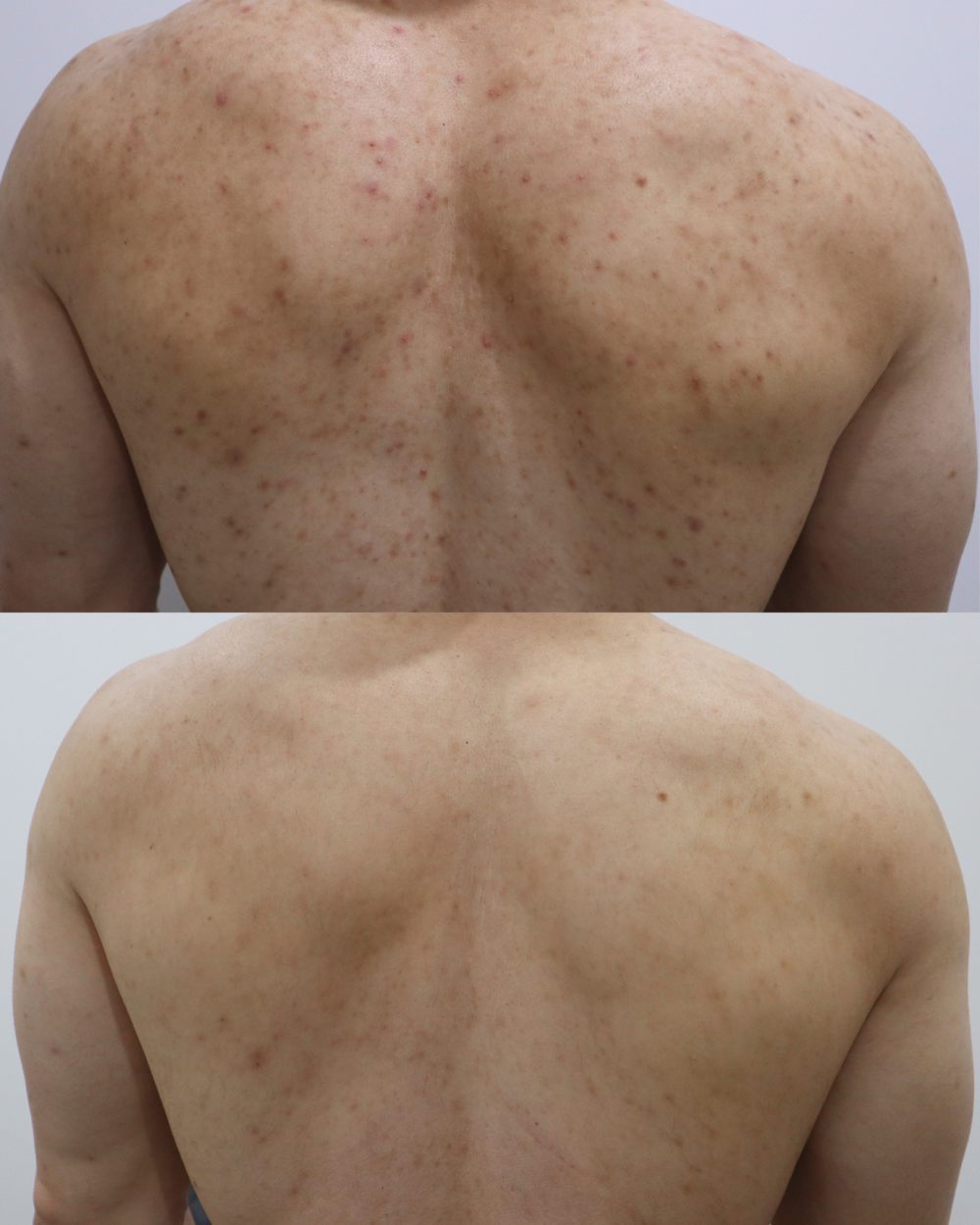
Acne
What is acne?
Acne, also known a zits or pimples, is a common skin condition that causes the sebaceous glands to become trapped with dead cells and oil.
People with acne tend to produce more oil.
Acne typically impacts almost 90% of teenagers according to the Australian Family Physician Journal*1 and often impacts many adults too.
Acne can cause devastating self-esteem issues, but the good news is that today there are many fresh options for people with acne.
People with acne tend to produce more oil.
Acne typically impacts almost 90% of teenagers according to the Australian Family Physician Journal*1 and often impacts many adults too.
Acne can cause devastating self-esteem issues, but the good news is that today there are many fresh options for people with acne.
What are the different types of acne?
Acne types include
Acne Vulgaris – By far the most common type of acne, considered mild acne or the type most commonly linked to “teenage pimples”.
Fungal Acne or pityrosporum folliculitis – This is a result of excess yeast in the hair follicles and skin may become itchy and red.
Nodulocystic Acne – This involves multiple inflamed cysts and nodules that can turn red or purple and scar.
Acne Conglobata – A rare, very severe form of inflammatory acne that results in often dome shaped nodules and large, interconnected pimples that bleed. More common in men.
Acne Fulminans – A sudden severe reaction that causes deep ulcerations and can be associated with joint pain and fever. Almost exclusively impacts adolescent males.
Acne Mechanica – Caused by pressure, friction or rubbing from clothing, masks or hats.
Infantile Acne – A type of acne common in babies driven by hormone surges. It typically clears up within the first year but if concerned see your doctor.
Acne Excoriee – Linked to anxiety and depression, driven by a compulsive urge to pick, scratch and squeeze acne scabs. Mainly affects young women.
Acne Cosmetica – Caused by (comedogenic) cosmetics and creams.
What parts of the body are most prone to acne?
Acne typically occurs on the forehead, face, upper back and shoulders.
What causes acne?
Acne is due to a combination of factors including:
- Genetic predisposition
- Hormones (typically in women there are flare ups before menstruation, and in men excess testosterone is the main acne trigger around puberty).
- Innate immune response
- Underlying disease such as Polycystic Ovarian Syndrome
- Some medications such as steroids, cortisone, lithium for bipolar disease and anti-convulsants*2
- Cosmetics that block the skin
- Stress, face masks or sweaty gym gear can also aggravate acne
What are the symptoms of acne?
- Open and closed non-inflamed comedones (blackheads or whiteheads)
- Inflamed papules (small, red, tender bumps) and inflamed pustules (papules with white pus on the tip)
- Cystic acne, which tends to be deeper in the skin, larger pimples that take longer to develop a white head
- Acne scarring – the fibrous process in which new collagen is laid down to heal a full thickness injury
- Scarring impacts more than one third of people with severe or moderate acne, and is most common in nodulocystic acne, acne conglobata and acne fulminans. To reduce your risk of scarring, treat your acne early and ask about our advanced laser treatments for acne scarring are read about them here.
- Acne is classified as mild or Grade 1 acne when there are occasional breakheads and a few papules and pustules.
- Grade 2 or moderate acne involves multiple papules and pustules mostly on the face, with a total body lesion count of <30.
- Grade 3 acne or moderately severe, nodulocystic acne involves numerous papules and pustules, along with occasionally inflamed nodules on the face. The back and chest may also be involved.
- Grade 4 or severe nodulocystic acne involves many large and painful inflamed pustules and nodules.
Should I pop a pimple?
Squeezing pimples can delay healing, lead to scarring or leave dark spots behind.
Picking at a pimple can also cause a serious infection.
Picking at a pimple can also cause a serious infection.
Does chocolate cause acne?
- There is much medical controversy about diet and acne.
- There is no solid evidence that chocolate or fried foods per se causes acne, though a low carbohydrate diet has been shown in some studies to improve acne.
- Foods that are thought to prevent skin inflammation are those high in omega 3 such as fish, eggs, kale, navy beans and walnuts.*3
How can I prevent acne?
- Wash your face with warm water only or a mild non-comedogenic (non-pore clogging) cleanser twice a day only.
- Always use a clean cloth.
- Avoid scrubs too often as this can lead to dryness and irritation, use no more than once or twice a month.
- Use products labeled “for sensitive skin”, these are generally more suitable than “deodorant soaps”.
- Use oil free sunscreen.
- Change your pillowcase twice weekly.
- Wash headbands and sports gear that can rub against skin and make acne worse.
- Pat rather than dry the skin after a shower.
- If your skin is oily, it’s best to avoid moisturisers all together. Otherwise use only fragrance-free, non comedogenic (non-clogging) moisturisers after you wash your face, and on the dry skin areas only.
- Be sun savvy. Sun can dry pimples out in the short-term but frequent excessive sun exposure causes the skin to dehydrate making the sebaceous glands produce more oil. This in turn can trigger more acne.
- Also ensure you are not dehydrated (thirst is the first sign of dehydration). Dehydration can make acne worse, along with alcohol, lack of sleep and stress.
What is the best way to apply acne medication?
- Always treat the whole area, rather than spot treat.
- Remember topical medications can initially dry out the skin so start using them every third or second day for a few weeks before graduating to every day.
- After a few weeks this sensitivity generally improves as your skin gets used to the medications. *5
- Be persistent. Sometimes one medication may not work in isolation, but may work when combined with another medication. Regular reviews with your skin doctor are important.
NOTE: For patients with persistent and severe acne, especially if there is concurrent bone pain or fever, a referral to a dermatologist should be requested urgently.